Practical Nursing Program Hands on Learning For Real World Impact
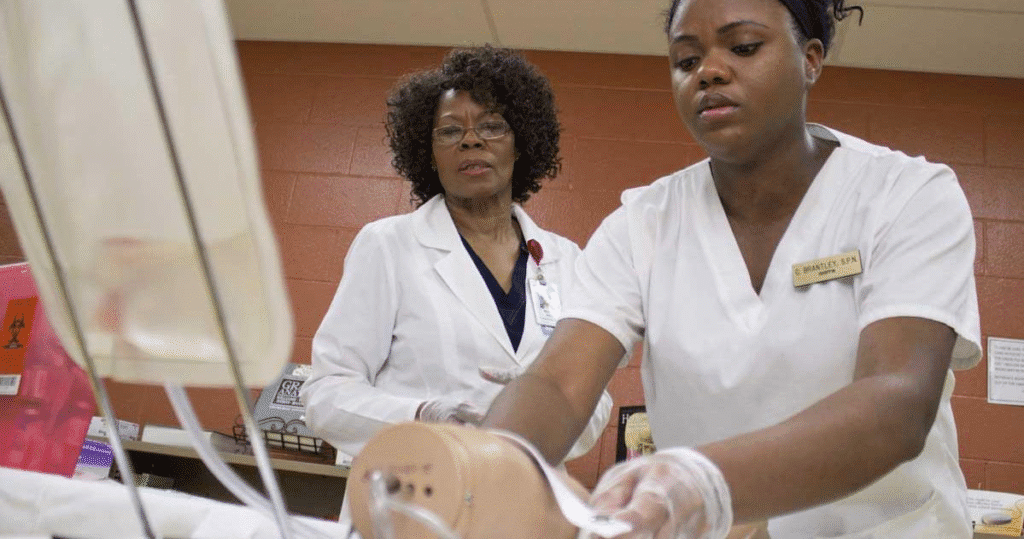
The healthcare industry today continues to seek skilled and caring nurses, leading to an acute need for individuals who can provide quality nursing care.The Practical Nursing Program represents a line of study for persons wishing to develop a nursing career that is an efficient, hands-on approach to obtaining education and experience. This type of program also must create a tie between the advanced classroom theory and the real clinical experience you will gain from the clinical practice, while giving students and aspiring nurses the knowledge, skills and attitude to be competent and confident to make a positive impact on the individual lives of patients. Experiential education is game-changing for preparing nursing students for real life practice in health care. It develops critical thinking, fosters empathy, and develops technical skill. Through simulated labs, monitored clinical experiences, and an interactive curriculum, students develop both the knowledge and the practical skills to thrive in any clinical environment. Building a strong foundation through applied education A vital element of the Practical Nursing Program is its emphasis on creating a solid foundation in the foundational principles of healthcare through applied education. Nursing students are introduced to a variety of essential concepts of nursing, such as anatomy, physiology, pharmacology, and patient care techniques. However, instead of having the student learn entirely in the classroom — the Practical Nursing Program places the classroom elements into practice through clinical experiences. This provides the nursing student with the opportunity to visualize how nursing concepts occur in real-life clinical cases. The collision of knowledge and experience ensures that practical nursing learners develop knowledge and competency. Clinical training The emphasis of the Practical Nursing program is clinical practice which provides the students the opportunity to gain supervised experience in hospitals, long-term care facilities, and other health care settings. By means of practical experience, students will learn about their responsibilities caring for patients, communicating with other health care professionals, and adjusting to the rapid pace of learning in the clinical environment. Greater awareness and understanding of different medical conditions as well as human feelings will result from their experiences with real patients. Developing professional and interpersonal skills The Practical Nursing Program is centered on the development of professional and interpersonal skills. Students are educated to communicate effectively with patients, families and members of the health care team. They are shown how to listen with empathy, provide support, and communicate their message in a way that is uncomplicated and clear. Each of these demonstrates critical communication skills an individual needs to build trust, as well as provide safe, quality nursing care. Professionalism is important in nursing education as students learn the ways in which to work collaboratively on an interprofessional team, develop leadership skills, and think in ethical ways. Students practice professionalism in their work by maintaining confidentiality, recognizing cultural similarities and differences, and advocating for the best interest of the patient. Simulation labs: Preparing for real-world scenarios Simulation laboratories create an experience that reflects a hospital setting and provide nursing students with a safe place to complete nursing skills. Nursing students can perform things such as wound care, catheter insertions, or emergency procedures using simulation scenarios. Simulation training provides an excellent opportunity for nursing students to build muscle memory for procedures they will eventually perform, as well as simulating what it feels like to remain calm, cool, and collected while in a stressful situation. Students are also given an opportunity to be comfortable making mistakes within the practice environment as mistakes are a part of learning. Critical thinking and decision-making in nursing practice The practical nursing program builds upon technical skills and develops critical thinking and good judgment. Nurses make decisions every day that impact patient outcomes. The program offers case studies, problem-based learning, and patient situations that require students to evaluate situations and respond in real time to develop thinking skills. In this way, the process allows students to evaluate symptoms, utilize data, and prioritize care in an efficient way. They will use both logic, empathy, and clinical thinking in every encounter Bridging the gap between education and employment An important advantage of the practical nursing program is that it can link education to employment because graduates are able to enter the workforce as soon as they finish the program. The practical nursing program hybrid model with classroom learning, a clinical placement and simulation labs prepares students in the qualities business is looking for when hiring in health care settings. The program teaches clinical skills and provides an understanding of workplace environments, documentation, and healthcare policies. The lasting impact of hands-on learning Experiential learning enhances nursing students’ attitudes to care deeply while creating a sense of fulfillment and motivation. Seeing the positive impacts of their own care ensures students understand the innate value of their roles. The emotional impact promotes engagement with nursing and enhances ongoing learning and development. Conclusion The practical nursing program prepares students for a rewarding life where they are knowledgeable, caring, and committed to serving others. With a focus on practical learning, graduates will learn and be confident to affect change in practice. Students gain the knowledge and competence to respond to a changing healthcare environment with care and expertise through clinical experiences, simulations and other methods of education.
Accelerated Practical Nursing Program Fast Track Your Future

The healthcare sector is one of the fastest-growing fields in the world, and the demand for qualified healthcare workers who have the education, training, and desire to provide compassionate and competent care to patients has never been greater. Licensed Practical Nurse (LPN) is one of the most significant professions in healthcare. LPNs are an important member of the healthcare team in hospitals, clinics, long-term care facilities, and community health. The accelerated practical nursing program allows students who are highly motivated to achieve licensure in less time by gaining the education and knowledge necessary to become employed. While the traditional educational path of practical nursing programs usually takes several years, accelerated programs generally employ a rigorous and intensive schedule to combine coursework, clinical experience, and professional preparation. Understanding the structure of accelerated practical nursing programs Accelerated practical nursing programs are developed to fit a traditional curriculum into a shortened period yet not cutting short the skill and knowledge attainment. Students should expect a more in-depth course of study, with classes, labs, and clinical rotations scheduled into shorter periods of time. This allows students to receive the same core education as those in traditional programs, covering all the necessary anatomy, physiology, pharmacology, and fundamentals of nursing courses. In addition to class time, students in the accelerated nursing programs practice hands-on learning in clinical training. Students are supervised by qualified instructors and practice direct patient care in real-world health care settings. This balance of lecture education and hands-on clinical training supports adequate education in theory, as well as confidence in performing the essential duties of nursing with a real-life patient. Benefits of choosing an accelerated nursing path A primary advantage of accelerated practical nursing programs is the possibility of a quick entry into the workforce. Rather than waiting two or three years to begin a career, graduates of an accelerated program typically can finish their course work anywhere from one academic year to eighteen months, depending upon the program. Therefore, these programs appeal to people who have a desire for employment and financial stability without having to wait for several years to pursue a job. Another advantage of an accelerated practical nursing program is the compact learning approach. Because this type of program is shortened, students are engaged directly in nursing education on a daily basis which frequently helps confidence retention of learning and the development of practiced skills. The consistent involvement of the students transforms into a solid foundation of knowledge and skills that provide the students with the skill set required as a licensed practicing nurse and for practical nursing in the care of patients. Choosing the accelerated program path ultimately reflects the urgent care shortage of nurses in today’s healthcare system. Students attending an accelerated program begin with an associate of science degree with an educational mindset that seeks out employment that is abundant and valuable reciprocally. There is always a pressing need for competent individuals in hospitals, clinics, and long-term care facilities and both current students and associates, typically find themselves entering into a future health career with an abundance of opportunity. Long-term career opportunities An accelerated practical nursing program is not only a fast track into the healthcare field but also a pathway to long-term career potential. A Licensed Practical Nurse can work in a variety of settings, from hospitals to private practices, and often a licensed practical nurse will later continue education and enroll in a bridge program to attain Registered Nurse (RN) status or a higher degree in nursing. The prep work from working through an accelerated program enables graduates to build experiences toward future careers and their professional development pathways. Graduates can either continue to do direct patient work or transition into a specialty area, taking with them the skills, discipline, and flexibility gained from the intensive education of a fast track nursing program. Meeting the needs of modern healthcare Contemporary healthcare systems depend on competent personnel who are responsive to patient needs in a timely manner. Accelerated practical nursing programs contribute to this demand by training competent graduates in a more timely manner. Because healthcare organizations are facing nursing shortages, the accelerated route is a timely solution for both students expecting a career and employers expecting necessary staff. This alignment of the educational process and the workforce demand is part of the reason accelerated programs have realized popularity. By balancing speed and quality, accelerated programs ensure that the healthcare system has a steady stream of qualified nurses contributing to the workforce. Conclusion Healthcare systems often depend on qualified people to respond rapidly to customer service needs. Accelerated practical nursing programs fill this demand by preparing capable graduates in a significantly shorter time. This offers an immediate solution to nursing staff shortages experienced by healthcare facilities and assists students, as soon-to-be graduates, in pursuing a desired career. The alignment between education and workforce demand is certainly part of the growth of accelerated programs. Education that combines speed with quality assures the healthcare system that qualified and competent nurses continue to enter the workforce to become productive members of the service arena.
Can Nurses Work Remotely?

Though older nurses tend to visualize bedside nursing when they think about nursing, now there exist all sorts of tele-nursing opportunities for working nurses with expanded roles beyond old-fashioned in-your-face, down-in-the-pits direct bedside contact with sick patients. Nursing practices have widened through telemedicine advances, expansion into health informatics, delivery as insurance healthcare services, and faraway remote monitoring of patients. Remote nursing presents an opportunity for licensed practitioners to increase their reach while reaping the rewards of flexible hours, decreased exposure to infectious diseases, and improved work-life balance. Remote nursing also assists in resolving the increasing healthcare worker shortage by accessing talent pools that may not be available for on-premises positions, such as rural-dwelling nurses or those working from home because of family commitments. Yet, remote nursing isn’t problem-free—it needs robust communication skills, technology literacy, and the ability to provide empathic care through a monitor or telephone. As telemedicine and online healthcare services expand, remote nursing is finding its place in the long-term future of the nursing industry. The emergence of remote nursing is primarily associated with the growth of telehealth services and the mounting application of digital technologies within healthcare. The rise of remote nursing Telemedicine platforms enable patients to meet with healthcare providers remotely and without going into a facility in person, and nurses are integral to these sessions. There were already increasing opportunities within telephone triage, nurse hotlines, and case management even before the pandemic. However the pandemic radically sped up the uptake of remote healthcare paradigms. Governments, insurance providers, and healthcare organizations moved rapidly, heavily investing in infrastructure capable of enabling remote consultations and observation. Consequently, several nurses shifted to jobs in which they could evaluate patients, offer health education, monitor chronic conditions, and even aid in basic diagnoses—all remotely. Remote nursing jobs today exist in a broad range of healthcare environments, from hospitals and insurance providers to telehealth companies and government initiatives. This change has opened up career paths for nurses, further diversifying the profession and making it more adaptable and robust in a changing world. While fundamental nursing skills like patient assessment, medical knowledge, and critical thinking are still required, remote nursing also requires a few more skills. Skills required for remote nursing Great communication skills are essential. As nurses are unable to physically examine patients, they have to depend heavily on patient descriptions, observation via video, and questioning in detail. The skill of being able to ask the appropriate questions and listen intently can make a huge difference in determining the right care path. Technical competence is also essential. Remote nurses need to be at ease with using electronic health records (EHRs), telehealth systems, and communication platforms such as Zoom or Microsoft Teams. Data security and patient confidentiality protocols have to be followed in a virtual setup. In addition, autonomous problem-solving abilities are essential. Remote nurses frequently work without the immediate physical backup of colleagues or supervisors. They need to be able to make decisions independently and recognize when to refer cases for additional medical intervention. Empathy and emotional intelligence are crucial. Establishing trust with patients over a screen or phone call demands real compassion and the ability to express care without physical presence. Benefits of remote nursing Remote nursing provides several important benefits for nurses and health systems. Remote positions tend to offer nurses more flexibility. Flexible working hours are often permitted, allowing for a more convenient balance of personal and work responsibilities. Flexibility can be especially attractive for nurses who have family responsibilities, are caregivers, or are living with their health conditions.Telecommuting also limits one’s exposure to workplace dangers such as contagious illnesses, on-the-job violence, or physical injuries due to overworking and over-lifting. Working at home may also bring about greater job satisfaction and sounder mental well-being since nurses are able to have a more relaxed and tailored workplace setting. For healthcare systems, the use of remote nurses can increase access to care, particularly in underserved or rural locations where access to healthcare providers is limited. It can also lower operational expenses since fewer resources are required for physical infrastructure and supplies. Challenges and limitations While it has its benefits, remote nursing also has its drawbacks. One of the main concerns is the lack of ability to perform physical exams. Certain conditions need to be touched, vital signs taken, or in-person diagnostic tests that cannot be done efficiently remotely. Technical issues are another frequent obstacle. Slow internet, software malfunctions, or unfamiliarity with telehealth systems can interrupt patient care and cause frustration for both patients and nurses. Remote nurses can feel isolated too. In contrast to a hospital where camaraderie and teamwork exist as a day-to-day component, working remotely can be lonely. Continuing education and maintaining professional relationships might need to take an extra step of effort. Furthermore, licensing and regulation can complicate remote nursing, especially for individuals who want to work across national or state borders. Nurses will need to have proper licensure to practice within the jurisdictions their patients are found in, often involving dealing with complex legal prerequisites. Future of remote nursing The future of distant nursing is bright, particularly with healthcare systems spending more on digital infrastructure and patients becoming increasingly used to virtual treatment. Emerging technologies like wearable health monitors, tele-diagnostic tools, and AI-powered triage tools will strengthen the skills of distant nurses. Educational curricula are starting to integrate telehealth training in nursing education, readying new nurses to practice in hybrid models of care with both in-person and virtual components. Policy reforms that enhance telehealth reimbursement and broaden interstate licensing compacts will also contribute to the development of remote nursing positions.Over the next few years, remote nursing will become an accepted component of healthcare delivery. Nurses who accept technology, pursue specialized education, and learn to accommodate new styles of communication will be well-positioned to excel in this new environment.
How Nurses Make A Difference Heartwarming Patient Stories

Nursing is considered one of the most noble and caring professions. Nurses, beyond giving medicine and checking vitals, offer emotional support, stand for their patients, and sometimes substantially alter lives in many ways beyond medical treatment. Their ability to build meaningful relationships and their attention to patient well-being makes them vital in the healthcare sector. By real-life accounts, we can see nurses’ everyday impact. A comforting presence in the final moments One of the most significant contributions nurses achieve is to provide dignity and solace to dying patients. Consider the narrative of Mary, a hospice nurse who took care of a senior cancer victim named Richard. With his condition deteriorating fast, Richard had no close family members. He mentioned his fear of perishing alone; Mary made it her goal to see that he never felt neglected. She reorganized her list of activities to be by his side, played his most loved music, and grasped his hand when he drew his last breath. Richard found peace in Mary’s presence, which reveals how important a nurse’s empathy can be under such circumstances. Going beyond the call of duty Nurses sometimes exceptionally aid patients beyond their job descriptions. Jessica, a pediatric nurse, encountered a young burn patient known as Liam. The crash left Liam traumatized and resistant to therapy. Seeing his pain, Jessica spent some time trying to connect with him. Knowing about his love of superheroes, she started including superhero-themed narratives and bandages into his daily care plan. Liam’s attitude improved over time and he started engaging in therapy. Her compassion and creativity aided him to recover not only physically but also emotionally. An advocate for the vulnerable Nurses often act as patient advocates, guaranteeing they get top-notch treatment. Sarah, an ICU nurse observed that her patient a comatose accident victim was being neglected in care decisions since he had no family around. Sarah decided it was her duty to advocate for a thorough check of his state. Working with experts, she organized debates, and at last, arranged a lifesaving operation. Later, the patient awoke to thank the nurse who had battled for him when he could not. Bringing joy to pediatric patients Nurses provide happiness to children in hospitals, happiness, and relief even though they feel scared and alone. A pediatric oncology nurse, Tom decided to dress up Friday as various Disney characters to cheer the kids up. Even through her most aggressive treatments, one young patient, Emily, who had been fighting leukemia, impatiently awaited his visits. Tom’s hard work transformed awful events into times of laughter, therefore showing that recovery is more than just physical treatment and also emotional support. Supporting families in difficult times Besides patients, nurses also assist families. NICU nurse Lisa dealt with a premature infant named Noah whose parents were terrified and unsure. Lisa patiently explains every step of Noah’s treatment and progress to help and console them. She went so far as to compile everyday notes into a little scrapbook so that they could follow their kid’s path. When Noah was discharged, his parents attributed their ability to care for him to Lisa. Resilience and dedication in crisis Nurses risk their health to look after patients throughout the COVID-19 epidemic. An ICU nurse, Emily remembers twelve-hour shifts, comforting patients who need to say goodbye to their families and serving as a surrogate family member for those quarantined because of the outbreak. An older patient, Mr. Miles, Thompson had no one present. Emily remained after her usual hours to sing his preferred songs and sit with him till he gently passed. Even under the most trying situations, her commitment shows the compromises nurses make for their patients. Encouraging recovery with compassion A nurse’s support can make a significant difference during a long and challenging rehabilitation process. Maria, a rehabilitation nurse, treated James, a stroke victim who could no longer walk. Feeling close to despair, James was frustrated and despondent. However, Maria refused to let him give up. She celebrated every milestone and set small, achievable goals, finding creative ways to keep him motivated. Thanks to Maria’s unwavering support, James eventually took his first independent steps after several months of hard work. Conclusion The foundation of the healthcare system is built on nurses, who provide care that goes far beyond medical treatment. Patients and their families find hope, comfort, and strength in them. Nurses make a significant impact, whether through small gestures or life-changing actions. Their stories reflect the kindness, dedication, and resilience that allow them to transform the lives of many people every day. Since they are often taken for granted, it is essential to recognize and appreciate the invaluable role they play in our lives.
How To Handle Difficult Patients And Families

The most challenging part of healthcare is handling difficult patients and their families. There are many cases of clients or family members being anxious, irritated, or even violent, no matter if you are a nurse, doctor, psychologist, or support personnel. Handling such circumstances well allows for a balance of empathy, communication abilities, and professional boundaries. Understanding why patients and families become difficult Before you handle challenging actions, it’s essential to know why they arise. Medical problems and results sometimes cause patients and their families fear, anxiety, discomfort, and doubt. This attitude can show anger, irritability, or skepticism of medical practitioners. Fear and anxiety: Uncertainty about diagnosis, therapy, or medical expenses might lead to increased feelings. Pain and discomfort: patients in pain can lash out irritably or hostilely. Lack of control: Feeling powerless in a medical circumstance can drive a requirement to assert control. Communication barriers: Misunderstandings arising from language, cultural variations, or medical terminology may irritate patients and their families. Previous negative experience: Patients or families with a history of poor healthcare experience could be mistrustful or belligerent. Understanding these triggers Strategies for handling difficult patients and families Maintain composure and professionalism. Remaining calm is essential when dealing with a disturbed family member or patient. Frustration or defensiveness can only make things worse. Instead: Respond after taking a deep inhalation. Maintain a constant and composed tone of voice. Keep an open posture and a neutral gaze. Practice active listening. Attentive listening can help to downplay emotions and indicate your sincere concern. Employ the subsequent methods: Keep eye contact to show interest. Nod and offer verbal affirmations. Restate what the individual is saying to verify the knowledge. Show empathy and compassion. Empathy can help one develop rapport and trust. Accept feelings by saying: “Let me see. It is a rather difficult period for you.”Let’s find a way to solve this collaboratively”. “I know it can be difficult to wait for outcomes”. “We’re trying our hardest to present the most precise data at the earliest possible moment”. Set boundaries and remain assertive. Although empathy is vital, keeping professional boundaries is even more important. When a patient or family member is demanding more or verbally abusing: Clearly define acceptable conduct and use statements like “I need you to talk politely so that we may have a good dialogue as I want to assist you”. Give honest and explicit information. Many disputes come from wrong perceptions. Keep the vocabulary straightforward and clear of technical terms. Offer written notes or screens when needed. Check comprehension by requesting the patient or family members to reiterate principal points. Involve the patient and the family in decision-making. Encourage the patient and their family to participate in decision-making. Encouraging patients and families in treatment choices will help patients: When feasible, provide options such as “Would you rather take your medication before or after your food?” Discuss treatment alternatives and seek opinions. Honor personal choices and cultural ideas. Employ de-escalation techniques for aggressive behavior. De-escalate the confrontation while putting safety first when a patient or family member is confronted. Stay calm and don’t take any offense. Give them space and prevent unexpected and sudden movements. Speak slowly and smoothly. Call for security if needed. Know when to get assistance. To provide comprehensive care, you may need assistance from: A director of a hospital or a manager A therapist or a psychoanalyst. Special considerations for different patient types Families and aged patients Be slow in your voice and be patient. Approach cognitive disabilities with empathy. Include relatives in conversations related to therapies. Patients with mental health issues Don’t judge; rather show empathy. Use soothing words and comfort to de-escalate. When needed, seek assistance from psychiatric experts. Non-native language patients and families Rely on professional translators rather than family members. Use visual aids or interpreted documents. Terminally ill families and patients Provide palliative care as well as emotional support. The prognosis should be handled honestly. Promote counseling or support groups. Self-care for healthcare professionals Dealing with challenging patients and families can be emotionally draining. Healthcare providers should give priority to self-care to avoid burnout. When possible, take occasional breaks. Approach difficult circumstances with colleagues or mentors. Participate in stress management exercises like meditation or exercise. If job stress starts to get unbearable, seek professional help. Conclusion Experts can effectively navigate difficult patients and families with the proper techniques. Healthcare professionals can build better patient connections while preserving their well-being by showing empathy, creating boundaries, and communicating precisely. Better patient outcomes are guaranteed by empathy and professionalism.
Common Nursing Mistakes And How To Avoid Them

A demanding career that requires responsibility, competence, and empathy is nursing. Nurses are indispensable to patient care. Often the first line of defense in spotting and managing possible medical issues. Sometimes, the demanding nature of nursing can result in mistakes that affect patient care and safety quality. Maintaining high standards in healthcare depends on knowledge of typical nursing errors and methods of avoiding them.The demands of the job, the fast-paced setting, and the emotional burden can cause errors. Nurses should always stay alert. To keep quality standards in healthcare, one must know typical nursing errors and how to avoid them. Through awareness of possible obstacles and use of best practices, nurses can improve patient results, lower liability, and create a more secure healthcare setting. Medication mistakes Medication errors are among the most frequent mistakes in nursing. Wrong dosages, wrong drug administration, or neglecting to look for drug interactions can all lead to this kind of mistake. How to avoid them Always respect the “five rights” of medication administration: the right patient, the right drug, the right dose, the right route, and the right time. Double-verify the labels and the medication prescriptions. Where possible, use electronic medication administration records (eMAR). Make sure all uncertain demands are addressed with the prescribing doctor. Keep abreast of possible drug interactions and medical knowledge. Errors in patient identification Administering therapy or drugs to the wrong person can be quite harmful. Busy hospital environments where nurses attend many patients typically have these mistakes present. How to avoid them Always utilize at least two patient identifiers: the patient name and date of birth. Before giving any medicine or healthcare, double-check patient information. Properly label every patient sample. Teach patients to point out problems they perceive. Failure to document properly Nursing depends on precise and promptly delivered documentation. Incomplete or inaccurate paperwork could result in legal problems and mistakes in inpatient treatment. How to avoid them Documents care promptly after using treatments or operations. Employ electronic health record systems and standardized charting formats. Stay clear and avoid using ambiguous terms. Re-examine documentation to make sure it is accurate. Inadequate communication Inadequate communication among doctors can cause patient injury, delayed therapies, and misinterpretation. How to avoid them Apply standardized communication tools, including SBAR (Situation, Background, Assessment, Recommendation). Attend team meetings from different disciplines and usual handoff notes. By restating main ideas, verify that the information given is grasped. Inspire team members to communicate freely. Lapses in infection control Healthcare-associated infections (HAIs) are a major concern in medical facilities and clinics. Preventing diseases’ spread depends hugely on nurses. How to avoid them Observe the hand cleanliness regulations strictly. Employ personal protective equipment (PPE) properly. Thoroughly sterilize and clean medical devices. Follow directions for wound care and catheter maintenance on infection control. Neglecting patient education Giving insufficient will cause patient noncompliance and bad consequences. How to avoid them Spare patients some time to learn about their medication, treatment strategy, and condition. When needed, use clear, nonmedical language and visual aids. Analyze understanding by having patients repeat the information back to you. Offer written guidance for home maintenance. Fatigue, burnout Long hours and stressful conditions are common among nurses and cause both physical and mental exhaustion. Fatigue raises the chances of mistakes. How to avoid them Give first attention to good rest and self-care. Give yourself intermittent breaks throughout your working day. Acknowledge burnout indicators and reach out for help when necessary. Support adequate staffing levels and flexible job hours. Neglecting pain assessment and management Inadequately evaluated and treated patient pain can cause extended agony and issues. How to avoid them Regularly evaluate pain with standard ratings. Record results of pain levels and pain management strategies’ impact. Talk to patients to learn their pain levels. Get familiar with treatment choices and pain management policies. Failure to prioritize care Competing demands on nurses could cause vital chores to be neglected. How to avoid them Cultivate excellent organizational and time management capabilities. Employ tools such as the ABC (Airway, Breathing, Circulation) technique to set priorities. Distribute tasks accordingly to other team members. Constantly evaluate patient needs throughout the shift. Conclusion Nursing errors can be avoided through proper awareness, training, and vigilance. Knowing typical mistakes and using best practices, nurses can offer more efficient and safer treatment. A successful nursing career depends on ongoing learning, good communication, and dedication to patient safety. Learning from mistakes and working for betterment is characteristic of committed and skilled nursing.
The Role Of Nurses In Pain Management

Nurses are involved in pain management, a fundamental part of medical care that directly impacts patient outcomes and quality of life. Whether acute or chronic, pain can affect somebody’s physical, mental, and emotional well-being. Nurses have a particular advantage as front-line medical providers in evaluating, observing, and treating pain using clinical knowledge, an empathetic approach, and patient education. Comprehensive pain assessment Thorough and clear evaluation is the foundation of good pain control and management. Nurses are trained in several means of pain evaluation that include patient self-reports, observational cues, and standardized pain assessment tools like the Visual Analog Scale (VAS), Numeric Rating Scale (NRS), and Wong-Baker FACES Pain Rating Scale. Identifying things that worsen or alleviate pain and acquiring data on the location, intensity, duration, and nature of the pain help to provide a thorough pain evaluation. It is very important to consider the emotional and psychological state of the patients. These factors greatly impact the recovery and pain-relieving process of the patient. Nurses should consider the cultural, social, and individual viewpoints of the patients to access thoroughly and provide quality care to the patient. To provide comprehensive care to the patients, nurses should know how to assess pain levels and provide pain management and care individually. Patient and family education Providing education to the patient and their family about pain management is an important responsibility of a nurse. Nurses empower patients and their families to make informed choices regarding their treatment by offering them knowledge on pain relief and pain management techniques. Some core educational topics may include: Medication usage: Proper dosage, possible side effects, and the importance of following prescribed schedules. Self-management skills: Instructing patients at home on non-pharmacological pain relief techniques. When patients should ask for help: Training patients to detect signals of poor pain management or drug side effects. Encouraging a collaborative attitude toward pain control helps nurses assist patients in actively engaging in their treatment, boosting satisfaction and results. Emotional and psychological support Patients need emotional and psychological support from nurses. Emotional support involves listening to patients’ fears, validating their experiences, and providing comfort. Building trust with the patient is the first step to alleviating suffering through good pain management. Nurses can refer patients showing depression or anxiety linked to constant pain to suitable mental health specialists and work with the medical group to treat these issues completely. Continuous monitoring and re-assessment Pain is a dynamic sensation that varies over time. To guarantee that pain management techniques remain effective, constant monitoring and re-evaluation are necessary. Continuous monitoring and ongoing evaluation are needed to guarantee the efficacy of pain control techniques. Nurses need to often assess the response to treatments, pain levels of the patient, and general advancement. The dynamic nature of a patient’s needs can mandate modifications to the overall approach to pain management. Another responsibility assigned to the nurse is the ongoing evaluation of the pain experience of a patient, monitoring the interventions put into effect, and overall progress. The pain management strategy might need adjustment depending on the changing needs of the patient. This process is critically dependent on documentation. Accurate and thorough documentation enables one to follow the impact of interventions and direct the next treatment choices. Furthermore, by enabling good communication among healthcare staff members, documentation guarantees continuity of care. Role in palliative and end-of-life care Pain control is a vital part of end-of-life and palliative care. Nurses in pain management provide compassionate pain control primarily for patients with terminal illnesses. This includes addressing physical pain as well as emotional and spiritual distress. It is the responsibility of palliative care nurses to know a variety of pain management techniques with the utmost clarity of ethical and cultural concerns that might impact end-of-life care. With their compassion and activity of consolation, they will enhance the quality of life of the patients and their family members. Pain relief techniques Physical therapies: Massage, heat and cold therapy, and directed exercises can all help to improve mobility and decrease discomfort due to pain. Applying cognitive-behavioral approaches: Mindfulness, relaxation techniques, and guided imagery can lower pain perception and improve coping skills. Complementary therapies: significant parts of pain management include acupuncture, aromatherapy, and music therapy. Conclusion Nurses offer a special combination of clinical knowledge, empathy, and patient advocacy, which is essential in the field of pain management. They offer thorough evaluation, non-pharmacological and medical therapy implementation, family and patient education, regular observation, and emotional support to patients for faster pain relief. Nurses are considered very important to ease pain and improve the general medical experience by using a holistic and patient-centered attitude. As healthcare evolves, nurses are considered a more significant part of the healthcare sector, emphasizing the need for continuous learning, training, and support.
Practical Nursing Pathways

Practical nursing is a critical and rewarding profession that gives essential care to patients in many healthcare environments. Depending on the state, practical nurses—known as Practical Nurses (PNs) or Vocational Nurses (VNs)—are essential for providing first-hand care and assisting registered nurses (RNs) and doctors. Educational pathways to become an PN. High school diploma or GED In order to enroll in any PN program, all applicants should possess at least a high school certificate or any equivalent General Educational Development (GED) credentials. Such a prerequisite education is aimed at fulfilling the PN program requirements in that it offers basic skills essential for proper functioning at an academic level, including English, math, and science, among others. Completion of an approved practical nursing program The most fundamental criterion for pursuing a career in PN is to successfully finish a government-recognized, practical nursing program. This program is usually found in community colleges and vocational and technical institutions. Such programs often take approximately 12 to 18 months to complete, leading to a diploma or certificate. Program curriculum The curriculum of practical nursing programs includes both theoretical classes and hands-on experience. Nursing Fundamentals: Introduction to basic nursing skills, ethics, and legal responsibilities in healthcare. Anatomy and Physiology: related to the study of internal structure and functions of the human body. Pharmacology: Basics of medications, dosage calculations, and safe administration techniques. Medical-Surgical Nursing: Training on handling common medical and surgical conditions in patients. Pediatric and Geriatric Nursing: Focused training on the care of children and elderly patients. Nutrition: Understanding the importance of proper nutrition in patient care and recovery. Mental Health Nursing: Basics of psychological care for patients with mental health conditions. Clinical practice or hands-on training In addition to theory delivered in classrooms, all state-approved PN courses provide practical training, which is also referred to as a practicum. The practicum involves hands-on work with patients in hospitals, clinics, and long-term care facilities. Clinical practice experience helps students gain different skills such as: Vital signs monitoring Wound care and dressing changes Administration of medications Patient hygiene assistance Basic patient assessments Pass the National Council Licensure Examination for Practical Nurses (NCLEX-PN). The National Council Licensure Examination for Practical Nurses (NCLEX-PN) is the exam necessary to acquire a license as a practical nurse (PN) or vocational nurse (LVN). Every nurse must pass this exam. It ensures that the candidates have the competencies required for safe nursing practices. State licensing requirements In every state, there is a board of nursing that oversees the licensing processes for practical nurses. Following the completion of their studies and passing the NCLEX-PN test, graduates are required to seek licensure from the relevant board in their respective states. Career opportunities for practical nurses Working in hospitals After completing a practical nursing program, most graduates will likely consider working in a hospital. In a hospital, PNs are expected to work with RNs and doctors in caring for the patients. Hospitals differ in the responsibilities that they assign to their PNs. However, PNs in a hospital setting can be expected to perform functions such as taking patients` vital signs, helping with basic care of the patient, giving medications, and working on the patient’s care with other nurses. Employment in nursing homes and long-term facilities PNs are mostly employed by nursing homes and long-term care facilities. Practical nurses in these settings continue to care for geriatric patients or patients with chronic illnesses who need assistance every day. Tasks range from aiding in hygienic operations, administering drugs, dressing wounds, or working/effective communication with other people in a medical setting to promote the health of the residents. Home healthcare Home health practice is quite simple for those who are used to the one-on-one mode of care. In this case, home health PNs make visits to the residences of the patients and offer the needed care, most commonly to nursing cases. Therefore, responsibilities help a patient with medication, carry out basic checks on the patient’s health, take care of the patient’s tights, and educate the patient and relatives on how the care would be. Outpatient clinics and physician offices Outpatient clinics and physician offices also hire PNs who help in patient care, usually in a more predictable, less hospital work-related setting. Duties of PNs in these types of positions can include, but are not limited to, taking patient histories, helping the patient prepare for an examination, injecting medications, drawing blood samples, and teaching the patient. Correctional facility nursing A career as a licensed practical nurse in a correctional facility can also prove to be an extremely demanding yet rewarding career for those seeking a challenging yet rewarding occupation. In most PN correctional facilities, basic health care services include medical assessments, administering pills by prescriptions, and emergency services to inmates. This is mainly because the majority of such establishments need a high amount of adaptability and safety awareness. Conclusion Practical nursing is a rewarding and versatile career path with many opportunities for advancement and growth. With educational and clinical training backgrounds, practical nurses are important team members in healthcare. With the ever-changing landscape of healthcare, PNs will continue to be an important link in the healthcare chain to provide optimal care and improve patient outcomes. For those who want to make a difference in other people’s lives, practical nursing pathways will provide an opportunity for this rewarding and promising journey.
Top skills you’ll learn in a practical nursing program

Practical nursing programs are very significant in providing successful and rewarding careers to practical nurses. These practical nursing programs are typically designed to provide skills and competencies to work as a practical nurse. These programs offer you numerous opportunities for advancement in your career. A practical nursing program should include every important aspect of working as an PN or RN. Academic coursework and hands-on training provided in these programs will help nurses in providing efficient and quality care to patients. The top skills you’ll learn in a practical nursing program are: Patient assessment and monitoring Patient assessment is the foundation of providing quality care to the patient. Patient assessment includes assessing the patient’s physical health along with collecting data related to the patient’s psychological and emotional health. Practical nurses learn how to monitor patients, take vital signs, and document issues. Patient assessment should be done effectively to respond to every health condition of the patient timely and rightly. During practical nursing programs, students learn how to: Assess symptoms Use diagnostic tools Monitor chronic conditions Clinical skills Clinical nursing skills are very important for practical nurses. Practical nursing programs provide clinical nursing skills that help nurses in providing direct patient care. Practical nurses should know about drug and medication dosage, dosage calculations, and drug interactions. Administering medication is the most significant task in practical nursing. Practical nurses should know about the patient’s issue rightly, and then they should also know about drug and medication dosage, dosage calculations, and drug interactions. Administering medications should be done safely. Proper wound care is important for promoting healing and preventing infections. Practical nursing programs teach students to clean, dress, and monitor wounds safely and effectively. Students also gain knowledge in infection control practices, such as proper hand hygiene, the use of personal protective equipment (PPE), and an understanding of infection transmission routes. Communication and interpersonal skills The practical nursing program includes different courses in communication and different workshops to gain expertise in effective communication. Effective communication skills are very essential while dealing with the patients. While working as a practical nurse, you may interact with patients daily and their families. So good communication skills are necessary. To understand patient needs and work with your team, you must have strong communication skills. To provide comprehensive care to patients, practical nurses should develop empathy and compassion. It also includes offering support to the patients. These qualities help in developing trust and building strong relationships with the patients. Technical skills Practical nurses should know how to use medical equipment. In practical nursing programs, they learn how to operate medical tools such as blood glucose monitors, infusion pumps, and electrocardiogram (ECG) machines. You should know the effective use of this equipment in providing quality care and treatments to the patients. Documentation and record-keeping lead to effective improvement in the patient’s health. Nurses should assess a patient’s health effectively and then document their collected data. Maintaining legal compliance and maintaining continuity of care depend on accurate and comprehensive documentation. Critical thinking and problem-solving A practical nursing program helps nurses develop critical thinking skills based on their assessments and observations. When students develop critical thinking and problem-solving skills, they can make informed decisions. Practical nursing programs allow nurses to complete several duties on schedule. Having good time management skills is essential in providing stress-free, timely service to patients. A practical nursing program teaches students how to prioritize tasks, manage multiple patients, and respond to emergencies effectively. Time management and organization skills include: Task prioritization Delegation Documentation Health promotion and education Practical nursing programs also emphasize the importance of health promotion. Students learn to develop and implement strategies to encourage healthy behaviors and prevent illness. This includes conducting health screenings, counseling on nutrition and exercise, and promoting vaccination and preventive care. Practical nurses should teach and educate patients about their health conditions, treatments, and lifestyle modifications. In practical nursing programs, students are trained in a way to provide clear, accurate, and personalized information to patients and their families. This involves teaching about disease prevention, medication management, and self-care techniques, which empowers patients to take an active role in their health. Adaptability Nurses should be prepared emotionally and physically to meet the needs of the practical nursing program. They may need to work for long hours in healthcare settings, dealing with critical situations of the patients. That’s why they should be emotionally and physically strong. Practical nurses should also develop effective strategies to manage these challenges and work effectively. They should always focus on their mental and physical health and maintain a healthy diet and lifestyle to keep their mind and body fresh. Practice yoga and meditation to relieve stress and take part in stress management techniques. Conclusion Practical nursing programs are designed to make sure that aspiring practical nurses are equipped with every essential skill to provide effective and comprehensive care to patients. Learning different skills will allow practical nurses to provide efficient services to patients. Engaging in continuous learning to keep up with the developments in the field is very important for the future and career development of practical nurses.
Nursing jobs for new graduates apply for entry level roles

The need for healthcare professionals is growing, and practical nurses are crucial to providing patient care in a number of settings. Graduates of the practical nursing program acquire important skills and knowledge that open up a variety of career opportunities. There are many roles for new nursing graduates to start their career. Shift from student to professional life is very significant for nursing students; therefore choosing the right career path is crucial for a successful and rewarding career. Students need comprehensive guidance on how to apply for entry-level roles and start their nursing career. Understanding entry-level nursing roles There are many entry-level nursing positions for new graduates who want to start their career. These roles and positions require basic nursing skills and knowledge about patient care. Students should also learn how to adapt to these nursing roles. Entry-level positions include: Registered nurse (RN) in hospitals Registered nurses are responsible for providing direct care to the patients, and they also coordinate and collaborate with healthcare professionals. They provide high-quality care to the patients in the hospital. They are also responsible for patient assessment and care, patient education, coordination of care, documentation and record-keeping, and patient and family support. Registered nurses acquire many skills, including clinical skills, critical thinking, and effective communication skills. Registered nurses work in hospitals, especially in surgical units and emergency departments. A Long-term care nurse Most common employment is working in long-term care facilities. It includes assisted living centres and nursing homes. Practical nurses tend to the needs of chronically ill patients and older patients in these settings. They are responsible for giving medication, helping with everyday tasks, keeping an eye on vital signs, and offering emotional support. Working in these facilities allows nurses to build good relationships and maintain their quality of life. It is a role that requires patience, and strong interpersonal skills. Outpatient clinic nurse These are the nurses who provide care to the patients who do not require hospitalisation. These nurses work in a variety of settings, including clinics, urgent care centres, and specialty practices. Their responsibilities, skills, and the environment in which they operate are distinct from those of inpatient nurses. Home health nurses For practical nurses who would rather care for patients in their homes as opposed to a clinical environment, home health nursing is becoming a more and more common employment option. In this setting, practical nurses help patients in their daily tasks, and also provide health education. Personalised and patient focused care is provided to the patients by home health nursing. In order to succeed in this sector, practical nurses need to be flexible, independent, and capable of handling a variety of medical situations. Public health nurse The specialty of public health nursing is centred on enhancing community health through outreach, prevention, and education. In order to promote healthy lifestyles, perform health screenings, and address public health issues, practical nurses in this field work in community clinics, public health organisations, and schools. Exploring various nursing settings There are a variety of healthcare settings where nurses can provide their services. New opportunities and experiences are provided in different healthcare settings. Hospitals For many new nurses, hospitals are the typical first place of employment. They provide a variety of patient groups, well-structured training programs, and the opportunity to collaborate with experienced medical professionals. Long term care facilities Working in nursing homes or rehabilitation centres provides experience in managing chronic conditions, treating different diseases, and building long-term relationships with patients. Outpatient clinics Often with a more regular schedule than hospital shifts, these settings provide the opportunity to focus on basic therapies and preventive care. Home health This role requires autonomy and strong time management skills, as you’ll be responsible for coordinating care for patients in their own homes. Utilizing job search platforms You can apply for jobs and find job opportunities using a number of online resources: Healthcare-specific job boards Nursing job postings and resources are the focus of websites like MedJobsCafe.com, AllNurses.com, and Nurse.com. General job boards A lot of jobs, including entry-level nursing positions, are listed on LinkedIn, Indeed, and Glassdoor. To focus your search on a certain area, kind of position, and other factors, use filters. Hospital career pages A lot of hospitals have specific career departments on their websites where you may apply for jobs that are available and find out more information about how they hire. Networking and professional development Social Media: Follow healthcare organizations, hospitals, and nursing groups on social media platforms to stay updated on job openings and industry news. Mentorship: Seek out experienced nurses who can offer guidance, support, and potentially even job leads. Mentorship can provide valuable insights into the profession and help you navigate the early stages of your career. Conclusion Starting a nursing career and acquiring entry-level positions is very important. You can choose the right role and position by focusing on diverse job settings, preparing thoroughly and effectively for interviews, and crafting a strong resume. Every phase of the entry-level role is a crucial aspect of a new nurse’s professional career because of the huge impact they have on patient lives and the healthcare system, which outweighs the initial challenges.
